Blocked Chest Tubes – Root Cause of Retained Blood
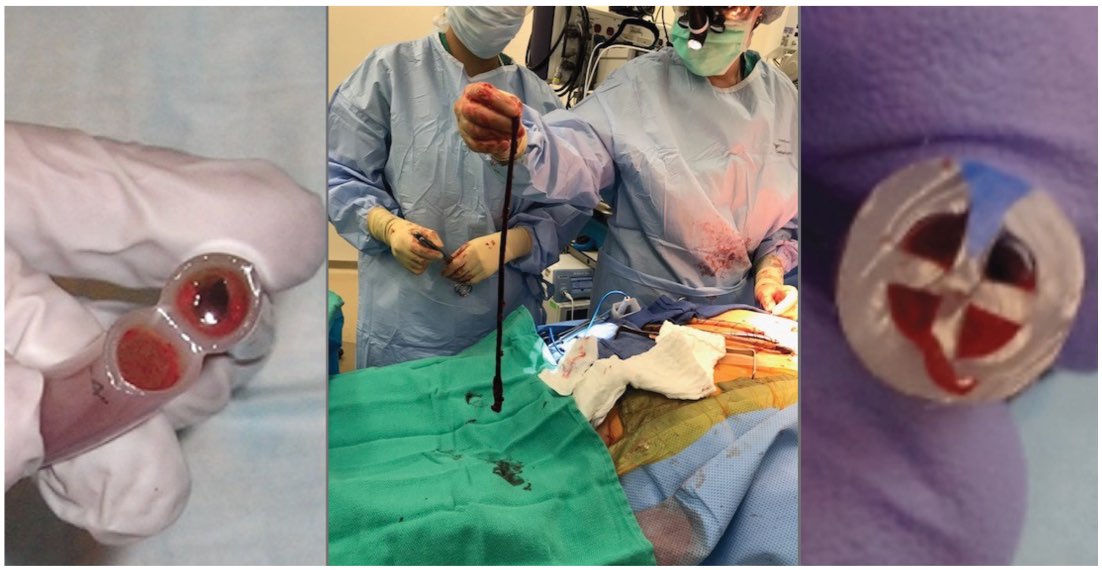
The crucial hours post-surgery make every bit of difference to the recovery of your patients. So why rely on a common chest tube to evacuate blood and fluids from a surgical site? Fact is, more than one in three cardiac surgery patients suffers from a blocked tube.
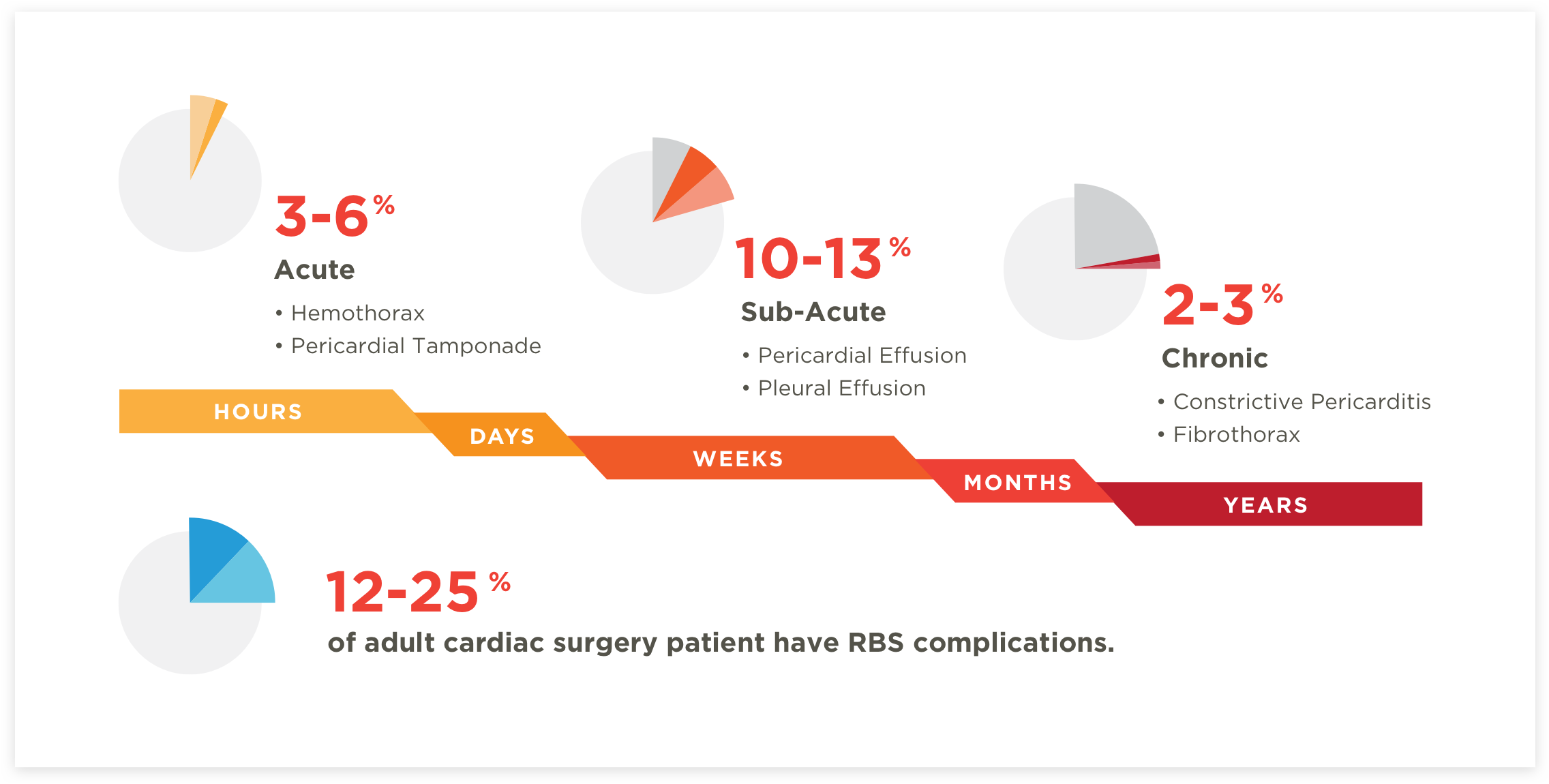
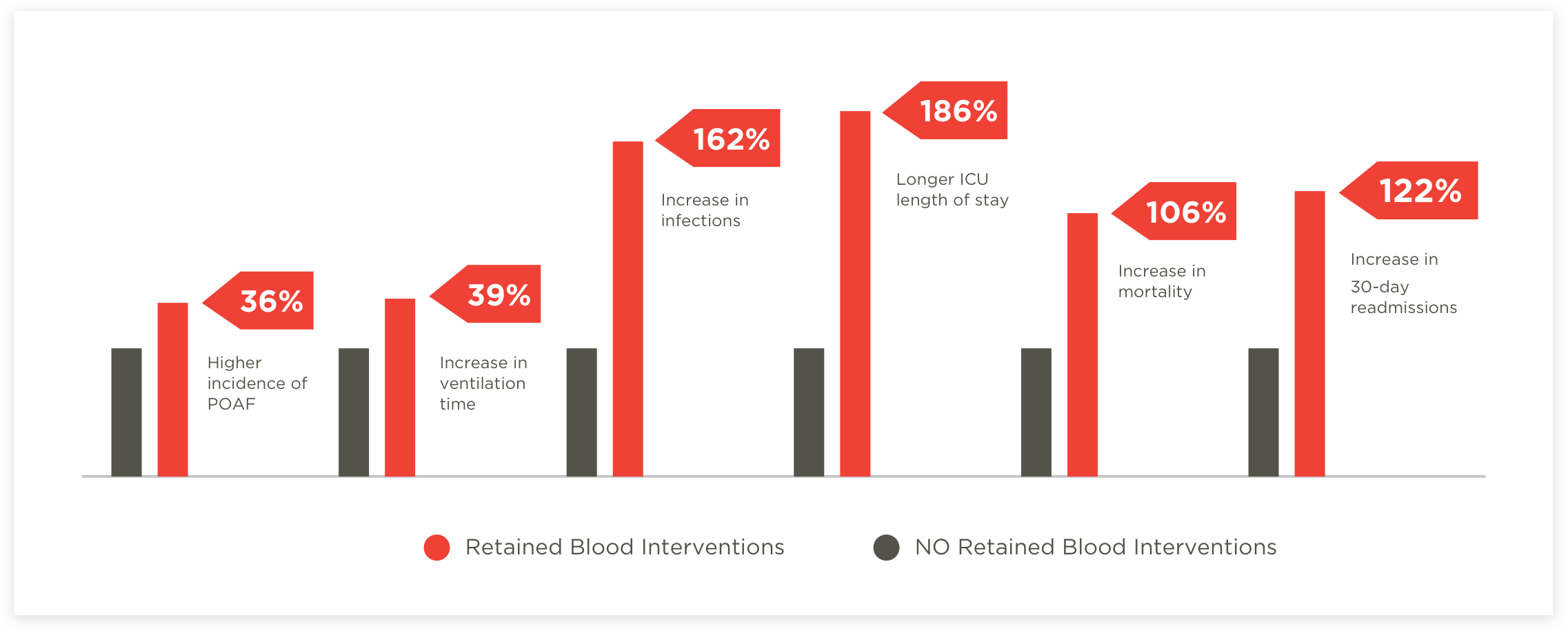
What’s worse, the majority of blockages are intrathoracic, therefore invisible to bedside providers. Failure to clear the catheter leads to adverse Retained Blood Syndrome (RBS) complications such as life threatening tamponade, pleural effusion, hemothorax, even infection due to tube manipulation.